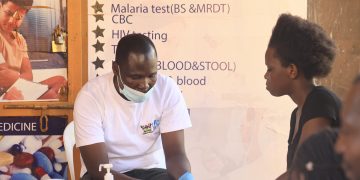
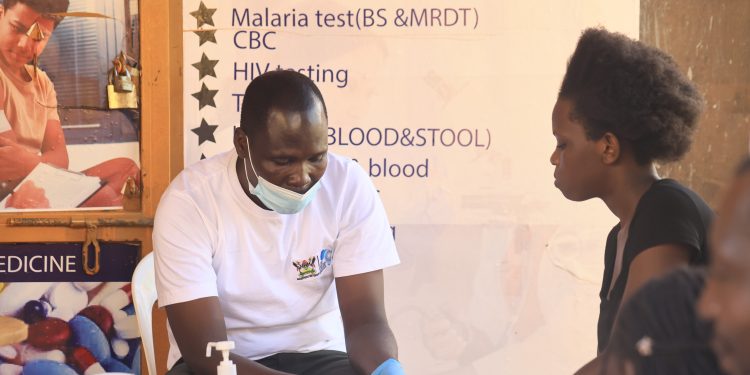
NSAMBYA, Uganda –During a fireside chat and mobile clinic outreach in Nsambya, a Kampala suburb, organised by the Uganda Youth and Adolescents Health Forum in partnership with Tiko Africa, health experts warned that survivors of sexual and gender-based violence (SGBV), especially young people, face serious mental, physical, and reproductive health risks if they do not receive urgent care.
Dr Okori Tom Felix, a medical clinical officer attached to Kisugu Health Centre, emphasised the importance of timely medical intervention following cases of sexual violence. A mobile clinic delivered critical services to residents of Nsambya, in Nsereko Village.
“When sexual gender-based violence occurs, these young people are psychologically affected, and in some cases, they sustain physical injuries. We must address both their mental health and physical condition,” he said.The mobile clinic, held at Top Medical Centre in Nsambya, aimed to expand access to youth-friendly health services within the community.
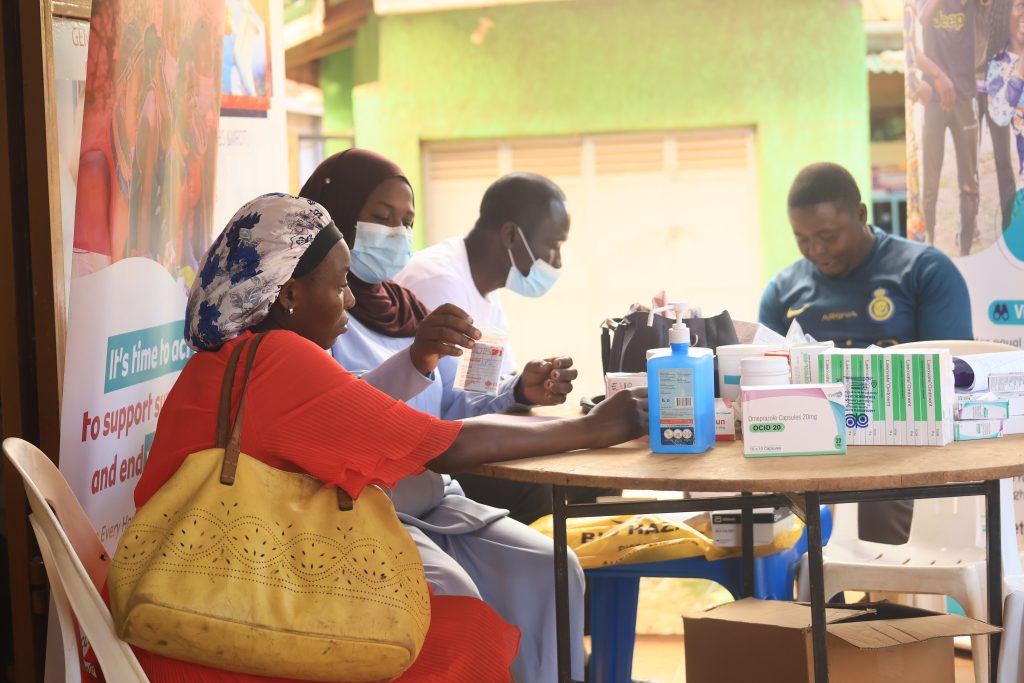 The mobile clinic, held at Top Medical Centre in Nsambya, Makindye Division aimed to expand access to youth-friendly health services within the community.
The mobile clinic, held at Top Medical Centre in Nsambya, Makindye Division aimed to expand access to youth-friendly health services within the community.
Dr. Okori explained that survivors of SGBV should seek medical help within 72 hours to access essential preventive treatment. These include post-exposure prophylaxis (PEP) to prevent HIV infection, emergency contraceptives to avoid unintended pregnancies, and antibiotics to guard against sexually transmitted infections.
“These services are time-bound. If a survivor comes within 72 hours, we can prevent HIV and pregnancy. Beyond that window, the risks increase significantly,” he noted.
He added that counselling and psychotherapy are also critical components of care, as many survivors experience trauma that requires professional mental health support.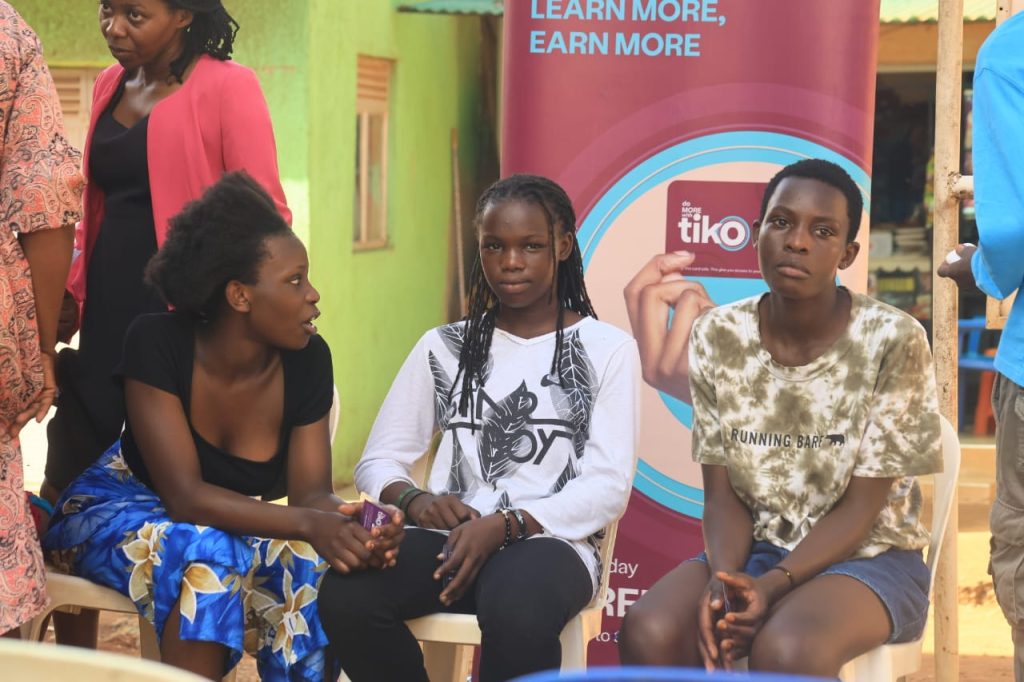 Beyond SGBV response, the outreach provided a range of sexual and reproductive health services, including family planning, HIV testing, and treatment for minor illnesses. According to Dr. Okori, at least 47 people were tested for HIV, with the majority being female. Additionally, several women received both short-term and long-term contraceptive methods.
Beyond SGBV response, the outreach provided a range of sexual and reproductive health services, including family planning, HIV testing, and treatment for minor illnesses. According to Dr. Okori, at least 47 people were tested for HIV, with the majority being female. Additionally, several women received both short-term and long-term contraceptive methods.
“We were able to offer family planning services to a number of young women and also treat common illnesses like respiratory and urinary tract infections using essential medicines,” he said.
Nora Nakyegera, Advocacy and Campaigns Officer at the Uganda Youth and Adolescents Health Forum, said the outreach was designed to address barriers that prevent young people from accessing health services.
“Many young people know about these services, but distance, lack of confidentiality, and fear of stigma discourage them from visiting health facilities. That is why we bring these services closer to them through mobile clinics,” she explained.
She added that the initiative also targets the “triple threat” affecting young people—teenage pregnancy, HIV infections, and sexual and gender-based violence—by combining service delivery with community awareness.
The outreach also featured a community “fireside chat,” where residents discussed key issues affecting adolescents, particularly sexual harassment and reporting mechanisms. Participants were sensitised on where to report abuse cases and the importance of seeking immediate help from health facilities and law enforcement. Community leaders welcomed the initiative, noting that it will improve access to free health services, including HIV testing and counselling.
Community leaders welcomed the initiative, noting that it will improve access to free health services, including HIV testing and counselling.
During the discussions, residents also addressed societal attitudes contributing to sexual violence. While some participants suggested that certain modes of dressing could provoke harassment, many women strongly rejected this view, insisting that no form of dress justifies abuse.
Health workers also used the platform to educate residents about HIV prevention methods such as pre-exposure prophylaxis (PrEP) and post-exposure prophylaxis (PEP), while encouraging the use of condoms.
Dr. Okori noted that some young people still feel shy about accessing condoms and other preventive services at health facilities.
“We encourage them not to feel ashamed. Condoms are freely available and help prevent both infections and unintended pregnancies,” he said.
Organisers say the mobile clinic model is proving effective in improving health-seeking behaviour among young people by reducing stigma, cutting transport costs, and bringing services directly into communities.
They are now calling for more partnerships to sustain such initiatives and expand outreach efforts to underserved areas.